Shared foundation
One application behind the evidence base
Teams work from one transparent application and adapt the evidence view to the question, audience, and decision stage.
Medip gives HEOR, market access, medical, commercial, and leadership teams a shared evidence base for different stakeholder questions.
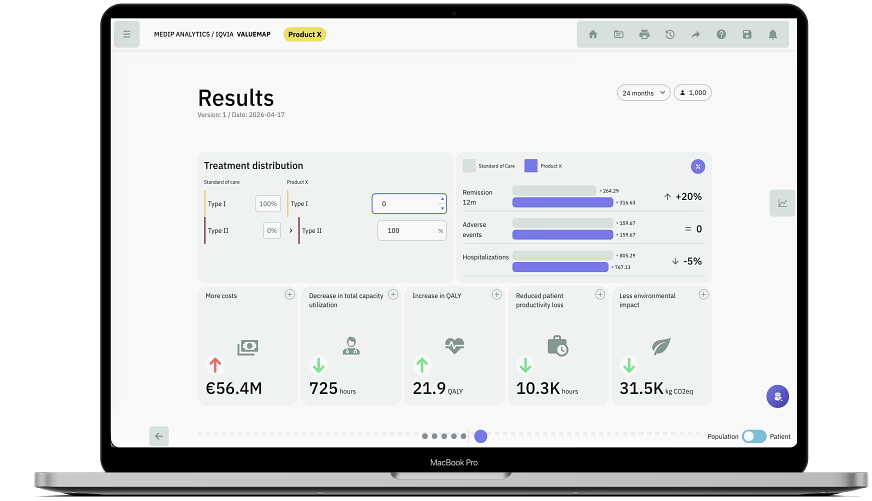
Keep teams aligned on the same evidence, assumptions, and pathway logic.
Give HEOR, market access, medical, commercial, and leadership teams relevant views.
Generate outputs for dossiers, publications, HCP discussions, payer cases, and launch planning.
Each team sees the part of the application that helps its decision, without losing the shared assumptions behind the result.
Develop transparent cost-effectiveness, budget impact, uncertainty, and scenario analyses from one application.
Turn technical evidence into reimbursement arguments, value dossiers, local adaptations, and payer-ready materials.
Explain how an innovation changes clinical decisions, patient outcomes, workflow, and downstream consequences.
Understand launch assumptions, pricing thresholds, eligible populations, adoption scenarios, and return on investment.
A single transparent application can reduce duplicated analysis, keep teams aligned, and make evidence easier to adapt across markets and audiences.
Shared foundation
Teams work from one transparent application and adapt the evidence view to the question, audience, and decision stage.
Local adaptation
Country, hospital, payer, and stakeholder settings can use different costs, populations, pathways, uptake assumptions, and comparators.
Evidence reuse
The same structure can feed value dossiers, reimbursement materials, publications, slide decks, hospital business cases, and internal decisions.
Ongoing learning
When new clinical data, prices, guidelines, or stakeholder questions emerge, the application can be updated and the model rerun.
Clinical, economic, operational, and broader value outputs trace back to the same pathway logic and assumptions.
Patient outcomes, survival, QALYs, avoided complications, treatment decisions, and diagnostic consequences.
Cost-effectiveness, budget impact, ROI, price thresholds, resource use, and downstream cost offsets.
Workflow, staff time, capacity, referrals, waiting lists, throughput, and implementation burden.
Productivity, caregiver burden, societal effects, environmental impact, and system-level consequences.

Join the discussion
We can map the outputs your HEOR, market access, medical, and leadership teams need from a shared evidence base.